Breastfeeding, a deeply personal and often challenging journey, presents a distinct set of considerations when viewed through the lens of neurodiversity. As understanding of autism expands, particularly regarding its presentation in women and its impact on family life, it becomes clear that traditional approaches to maternity and infant care may not adequately serve autistic parents or those breastfeeding autistic children. This article delves into the multifaceted experiences surrounding breastfeeding within the autistic community, highlighting both the unique strengths and the specific support needs that arise.
Autism Spectrum Disorder (ASD) is a neurodevelopmental difference characterized by variations in social interaction, communication, and patterns of behavior or interests. Autistic individuals, often described as neurodivergent, experience and interpret the world uniquely. This spectrum-based understanding means that each autistic person’s abilities and challenges are highly individual and can fluctuate depending on their environment and internal state. While awareness of autism has grown, particularly in children, a significant proportion of the adult autistic population, especially women, remains undiagnosed, complicating access to appropriate support during critical life stages such as parenthood.
The Landscape of Autism and Parenthood
Current estimates suggest that approximately 0.82% of the population in England are diagnosed with autism. However, a staggering 72% of the autistic population in England is believed to be undiagnosed, a statistic that underscores a critical gap in identification and support. This prevalence of undiagnosed autism, particularly among women, means that many parents navigate the complexities of maternity and breastfeeding without a formal understanding of their neurodivergent needs. The implications for healthcare providers are profound: a one-size-fits-all approach to maternity and breastfeeding support will inevitably fall short for a substantial segment of the population. Autistic women and parents may require highly individualised care, tailored to their unique sensory, communication, and emotional profiles.
Breastfeeding for Autistic Parents: Strengths and Challenges
The journey of breastfeeding for an autistic parent can be marked by both profound strengths and specific challenges. Many autistic women who choose to breastfeed report finding the experience a source of calm and empowerment. It offers a protected period of quiet connection, a respite from an often overwhelming world, which can be deeply satisfying and regulating. This positive experience is often bolstered by a characteristic autistic trait: a propensity for deep research and determination. Autistic individuals who decide to breastfeed often meticulously gather information, becoming highly knowledgeable and resolute in their feeding goals. This dedication can be a powerful asset in overcoming obstacles.

However, the broader context of maternity care and societal expectations can pose significant hurdles. Autistic women often mask their neurodivergent traits, suppressing their authentic behaviors to conform to neurotypical norms, even when they are in desperate need of support. This masking can make it difficult for healthcare providers to recognise their unique needs, leading to misinterpretations or a lack of appropriate interventions.
Communication Differences and Accessing Support
Communication differences are a hallmark of autism, and these can significantly impact an autistic parent’s ability to seek and receive breastfeeding support. These differences are often situational; an autistic person might be non-verbal in high-stress environments, yet verbally articulate in familiar, calm settings. This variability necessitates a flexible approach to communication in healthcare settings. Offering a range of communication methods – from written forms, typing on a phone, or using picture cards, to sign language – can be crucial. The ability to communicate effectively, without pressure or judgment, is fundamental to building trust and ensuring needs are met.
Traditional avenues for breastfeeding support, such as local groups or national helplines, can present formidable barriers. The social dynamics of group settings, the uncertainty of what to expect, and the potential for sensory overload can trigger anxiety. Many autistic women find it difficult to ask for help, a challenge exacerbated by prior experiences of feeling unheard or misunderstood within healthcare systems. This difficulty is compounded by the fact that some autistic mothers may struggle with phone calls, a common method for accessing national helplines or local services. Organisations like La Leche League (LLLGB) are beginning to adapt by offering alternative support channels, such as written help forms, which can significantly improve accessibility.
Furthermore, a higher incidence of Post-Traumatic Stress Disorder (PTSD) has been observed in the autistic community compared to neurotypical individuals. This statistic highlights a heightened vulnerability, particularly in the context of childbirth and early parenthood, where experiences can often feel disempowering or overwhelming. A lack of control over their bodies and experiences post-birth can compound existing vulnerabilities, making empathetic, trauma-informed care essential.
Sensory Differences: A Central Consideration
Sensory processing differences are a core aspect of the autistic experience, profoundly influencing how individuals interact with their environment. Autistic parents may experience heightened or reduced sensitivities to smell, taste, touch, sight, and sound, all of which can affect the breastfeeding experience. For example:

- Touch: The sensation of a baby latching, the feeling of milk let-down, or the constant skin-to-skin contact might be overwhelming or, conversely, a source of comfort. Certain fabric textures or clothing against the skin during feeding could also be distracting.
- Sound: A baby’s cries, suckling noises, or even ambient sounds in a feeding environment might be intensely amplified or distracting.
- Sight: Bright lights, cluttered environments, or even direct eye contact during feeding could be overstimulating.
- Smell/Taste: The natural scent of a baby, breastmilk, or even strong food smells nearby could be challenging.
- Interoception: Difficulties in perceiving internal bodily signals like hunger, thirst, or fullness can impact a parent’s ability to recognise their own needs or interpret their baby’s cues accurately.
Understanding these sensory variations is paramount for providing effective support. Creating calm, predictable, and sensory-friendly environments for feeding and support sessions can make a significant difference. This could involve dim lighting, quiet spaces, clear visual schedules for group meetings, and respecting personal space.
Breastfeeding an Autistic Child: Unique Dynamics
While adult autism diagnoses are often delayed, autism diagnosis rates in children are on the rise, increasing awareness of neurodivergent needs from an early age. The World Health Organisation recommends breastfeeding for two years and beyond, with the natural age of weaning estimated between 2.5 and 7 years. For an autistic child, or one suspected of being neurodivergent, breastfeeding can hold profound importance, extending beyond nutrition to encompass comfort, regulation, and a consistent source of sensory input.
Sensory Differences in Autistic Children and Feeding Patterns
Autistic children process sensory input differently, often exhibiting either heightened sensitivity (sensory aversion) or a strong need for specific sensory experiences (sensory seeking). These differences directly influence feeding patterns:
- Regulation and Comfort: Breastfeeding can serve as a powerful self-regulation tool for autistic children. When overwhelmed by sensory input from a busy, loud, or unfamiliar environment, a child may seek the familiar comfort and close physical contact of breastfeeding to calm themselves. This can lead to frequent, intense feeding, particularly in challenging situations.
- Aversion to Input: Conversely, sensory overload can make feeding difficult. A child might struggle to latch or feed if they are sensitive to the temperature of the room, the texture of clothing, or distracting sounds. Identifying and mitigating these sensory triggers is crucial.
- Interoception Difficulties: Like autistic adults, autistic children may struggle with interoception, making it hard for them to accurately perceive hunger, thirst, or fullness cues. This can lead to either infrequent feeding or overfeeding, and requires careful observation from the parent.
High-Needs Babies and Intensive Attachment
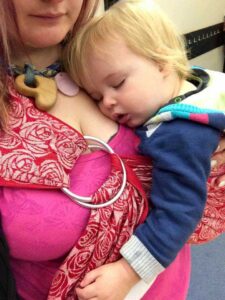
Many babies are described as "high needs," requiring intense closeness and frequent attention from their primary caregiver. This is a normal developmental phase, but it can be particularly pronounced in neurodivergent children. For autistic infants, the need for proximity, touch, and comfort provided by breastfeeding can be exceptionally intense. This can be physically and emotionally demanding for parents, underscoring the vital importance of robust social support from family, friends, and like-minded communities. Prioritising self-care becomes not just advisable, but essential for parents navigating these intensive early years.
Feeding Patterns, Boundaries, and Weaning
As autistic children grow into toddlerhood and beyond, frequent breastfeeding can become more challenging for parents. Weaning, a natural progression for all children, can present unique difficulties for autistic children due to sensory issues, communication differences, and the central role breastfeeding plays in their co-regulation and comfort. Children may struggle to transition to solid foods due to specific aversions to textures, tastes, smells, or even the visual appearance of food. This can result in an increased reliance on breastmilk for nutrition and comfort, extending the breastfeeding relationship beyond typical developmental milestones.
For parents, establishing gentle boundaries around feeding can be complex when communication is a challenge. Options for parents seeking to limit or stop breastfeeding include:
- Visual Schedules: Using pictures or simple visual cues to indicate when breastfeeding is available and when it is not.
- Distraction and Redirection: Offering alternative comforting activities or engaging distractions when a child seeks to feed.
- Verbal Cues (if applicable): Using consistent, simple phrases to signal feeding times or limits.
- Gradual Reduction: Slowly reducing the number or length of feeds over time, allowing the child to adjust.
- Alternative Comforts: Introducing other forms of comfort, such as cuddles, stories, or special toys, to replace breastfeeding as a primary regulatory tool.
It is important to acknowledge that many mothers choose to continue breastfeeding until their child self-weans, or they may responsively breastfeed older children on demand. Continuing to breastfeed into toddlerhood and beyond offers numerous benefits, including ongoing nutritional support (especially if a child has a limited diet due to sensory aversions) and continued emotional and regulatory comfort. However, the decision to set boundaries or wean is deeply personal, and parents of autistic children may require tailored support from lactation consultants or LLL Leaders who understand these specific challenges.
Implications for Healthcare Professionals and Support Systems
The insights gained from understanding the intersection of autism and breastfeeding carry significant implications for healthcare professionals and support organisations. A fundamental shift towards neurodiversity-affirming care is essential. This means moving beyond a deficit-based model to recognise and respect neurodivergent ways of being, adapting services to meet diverse needs rather than expecting individuals to conform to neurotypical standards.
Key considerations for supporting an autistic person to breastfeed include:

- Individualised Care Plans: Recognising that each autistic person’s experience is unique and requires a personalised approach.
- Sensory-Friendly Environments: Offering quiet spaces, managing lighting, and minimising overwhelming stimuli during appointments or support groups.
- Flexible Communication Methods: Providing options beyond verbal communication, such as written information, visual aids, or allowing a support person to communicate on behalf of the parent.
- Clear and Direct Information: Presenting information concisely, avoiding jargon, ambiguity, and excessive social nuances.
- Respecting Autonomy: Empowering parents to make informed decisions about their feeding journey, acknowledging their expertise in their own bodies and their child’s needs.
- Trauma-Informed Approach: Being aware of higher rates of PTSD and ensuring care is delivered with sensitivity, empathy, and a focus on consent and control.
- Training and Education: Equipping midwives, health visitors, lactation consultants, and breastfeeding peer supporters with comprehensive knowledge of autism and neurodiversity.
Organisations like the Maternity Autism Research Group (MARG) are vital in driving this understanding and advocating for improved maternity care for autistic individuals. The provision of accessible, empathetic, and informed support is not just a matter of best practice, but a fundamental right for all parents.
Conclusion
The journey of breastfeeding, whether as an autistic parent or in nurturing an autistic child, is a testament to resilience, adaptability, and the profound bond between parent and child. By acknowledging the unique strengths, navigating the specific challenges, and implementing neurodiversity-affirming practices, healthcare systems and support networks can ensure that all families receive the compassionate, effective care they deserve. This ongoing evolution in understanding and support will not only enrich the breastfeeding experience for autistic families but also foster a more inclusive and empathetic approach to parenthood for everyone.

