The intersection of autism and breastfeeding presents a multifaceted landscape of both distinct strengths and specific challenges, demanding tailored support and a deeper understanding from healthcare providers and support networks. Autism, a neurodevelopmental difference influencing how individuals experience the world and communicate, affects an estimated 0.82% of the population in England, with a significant proportion—up to 72%—believed to be undiagnosed, particularly among women. This critical data point underscores the hidden needs within the maternal and child health sector, where many autistic women and parents embark on breastfeeding journeys, and a growing number of breastfed children are identified as autistic. Recognizing and addressing these unique dynamics is paramount to fostering inclusive and effective breastfeeding support.
Understanding Autism and its Impact on Parenthood
Autism is characterized by a spectrum of presentations, meaning abilities and challenges vary widely among individuals and can fluctuate depending on environmental factors. This neurodivergence affects sensory processing, communication styles, social interaction, and executive functions, all of which can profoundly influence the experience of pregnancy, childbirth, and early parenthood, including breastfeeding. The diagnostic landscape for autism has historically been biased, leading to underdiagnosis in women who often develop sophisticated coping mechanisms, known as "masking," to suppress autistic traits in social situations. This masking can make it difficult for healthcare professionals to identify their needs, even when they are actively seeking support.
The journey of an autistic parent often begins with navigating maternity care, where standard protocols may inadvertently create barriers. For instance, environments that are overstimulating (bright lights, loud noises, strong smells) can be overwhelming due to sensory sensitivities. Communication differences can also pose significant hurdles; an autistic person might struggle with verbal communication in stressful situations or find it challenging to articulate their needs in typical conversational formats. These factors, combined with a potential history of feeling misunderstood or having limited control over their bodies and experiences, contribute to higher rates of conditions like Post-Traumatic Stress Disorder (PTSD) in the autistic community compared to neurotypical individuals.

Breastfeeding for Autistic Parents: Strengths and Challenges
For many autistic women and parents, breastfeeding is not just a biological function but an experience imbued with unique personal significance. While challenges exist, there are also notable strengths that can facilitate a positive breastfeeding journey.
The Calming Embrace and Empowerment:
Many autistic mothers report finding the act of breastfeeding deeply calming and enjoyable. It provides a protected time for quiet rest and intimate connection, acting as a sensory anchor amidst the often chaotic early days of parenthood. This consistent, predictable interaction can be particularly reassuring. Furthermore, successfully breastfeeding can be an empowering experience, offering a sense of achievement and control over their bodies and parenting choices, particularly significant for those who may have felt disempowered during other stages of maternity care.
Research Acumen and Determination:
Autistic individuals often possess exceptional abilities in focused research and independent information gathering. Parents who choose to breastfeed may therefore arrive with a wealth of knowledge, having meticulously studied the process, its benefits, and potential challenges. This dedication often translates into a strong determination to succeed, serving as a powerful intrinsic motivator. However, this depth of knowledge can also be a double-edged sword; if their experiences deviate from the "textbook," it can lead to increased anxiety or a feeling of failure if not adequately supported.
Navigating Communication and Support Systems:
Communication differences are a key area where support systems need adaptation. Recognizing that an autistic person may not always be able to verbally express their needs, especially under stress, is crucial. Healthcare providers and support groups should offer diverse communication methods, such as written forms, typing on a phone, visual aids like picture cards, or even sign language. The La Leche League Great Britain (LLLGB) offers a valuable service with its written "Help Form," demonstrating a proactive approach to inclusive support.

Traditional breastfeeding support groups, while beneficial for many, can be overwhelming for autistic parents. Unfamiliar environments, unstructured social interactions, and the expectation of verbal participation can be significant barriers. Strategies to mitigate this include providing clear visual guides on what to expect at a group, offering the option to attend with a trusted support person, and fostering a welcoming atmosphere that respects individual comfort levels regarding participation. The inherent difficulty many autistic women face in asking for additional support, often due to masking or anxiety, necessitates a proactive and empathetic approach from support providers.
Sensory Considerations in Breastfeeding:
Sensory differences are central to the autistic experience and profoundly impact breastfeeding. These differences can manifest as heightened or reduced sensitivity to touch, taste, smell, sight, and sound.
- Touch: The feel of a baby latching, the sensation of milk let-down, or skin-to-skin contact might be intensely pleasant or, conversely, highly aversive. Some might find the sticky feeling of milk uncomfortable, while others might crave the deep pressure of a baby nursing.
- Sound: The sounds of a baby feeding, suckling, or crying could be soothing or incredibly irritating. Noisy environments can disrupt feeding sessions.
- Sight: Bright lights, cluttered spaces, or even eye contact might be distressing. A calm, dimly lit feeding environment can be beneficial.
- Smell: The scent of breast milk, baby, or even personal hygiene products can be very strong, either comforting or overwhelming.
- Taste: While less direct for the parent, the taste of foods consumed might affect milk flavor, which could be a factor for sensory-sensitive babies.
For support providers, understanding these potential sensory sensitivities means offering practical suggestions: adjusting lighting, minimizing noise, ensuring comfortable clothing, and discussing positions that optimize comfort and minimize unwanted sensations.
Key Principles for Supporting Autistic Parents:
Supporting an autistic parent requires an individualized, flexible, and trauma-informed approach.
- Respect Autonomy: Always prioritize the parent’s choices and preferences.
- Clear, Direct Communication: Avoid jargon, metaphors, or implied meanings. Be explicit and factual.
- Sensory Awareness: Ask about sensory preferences and help create a comfortable feeding environment.
- Flexible Support Options: Offer various ways to access help (written, virtual, one-on-one).
- Patience and Understanding: Recognize that processing information or responding might take more time.
- Validate Experiences: Acknowledge their challenges and strengths without judgment.
- Address Masking: Be aware that a parent might appear fine even when struggling significantly.
Breastfeeding an Autistic Child: A Nurturing Connection
While adult autism diagnoses often remain elusive, diagnosis rates in children are steadily increasing, leading to a greater awareness of neurodivergence in infants and toddlers. The World Health Organization (WHO) recommends breastfeeding for two years and beyond, with the natural age of weaning estimated between 2.5 and 7 years. For an autistic or neurodivergent child, breastfeeding can be particularly significant, serving as a powerful tool for regulation, comfort, and nutritional support, albeit with its own set of considerations.
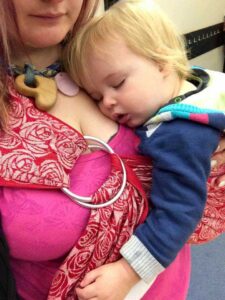
Sensory Processing in Autistic Children:
Autistic children often experience sensory input differently, which can manifest as either seeking out specific sensations or actively avoiding them. This can directly influence breastfeeding patterns:
- Seeking Behavior: A child might breastfeed very frequently to self-regulate when feeling overwhelmed or overstimulated. The rhythmic suckling, close physical contact, and comfort of nursing can provide a deep sensory input that helps calm their nervous system, especially in busy, loud, or unfamiliar environments.
- Avoiding Behavior: Conversely, certain sensory inputs might make feeding difficult. This could be anything from the temperature of the room, the texture of a parent’s clothing, specific smells, or even the feeling of their own socks. If a child struggles to feed, identifying and modifying the challenging sensory input can be crucial. Creating a quiet, dimly lit, and predictable feeding space can often facilitate successful nursing.
The "High Needs" Neurodivergent Child:
Many babies are described as "high needs," characterized by an intense desire for proximity and comfort from their primary caregiver. This is a normal developmental phase, but it can be particularly pronounced and prolonged in neurodivergent children. Their heightened sensory sensitivities, difficulty with transitions, and need for co-regulation can lead to more frequent and intense demands for breastfeeding and physical closeness. This intensity can be physically and emotionally draining for parents, underscoring the vital importance of robust self-care, a strong support system from family and friends, and connecting with like-minded communities.
Feeding Patterns, Boundaries, and Weaning Challenges:
As autistic children grow into toddlerhood, frequent feeding can become a significant challenge for parents. Weaning, a complex developmental process for any child, can be particularly challenging for autistic children due to sensory processing differences, communication barriers, and the critical role breastfeeding plays in their co-regulation and emotional security.
- Sensory and Interoception Difficulties: Some autistic individuals experience interoception difficulties, meaning they struggle to recognize internal bodily cues like hunger, thirst, or fullness. This can lead to either missing hunger cues or feeding past satiety. For children, this might mean they rely on breastfeeding as a primary food source, even when solid foods are introduced.
- Food Aversions: As they get older, autistic children may develop strong aversions to certain solid foods based on texture, taste, smell, or appearance. This can result in a limited diet, making continued breastfeeding essential for providing crucial nutrients they might otherwise miss. In such cases, an increase in breastfeeding frequency might be observed.
While many mothers choose to continue breastfeeding until their child naturally self-weans, or to nurse responsively on demand, others may need to set gentle boundaries or limit feeding frequency and duration. This can be especially difficult when communication issues are present. Support from an LLL Leader or other knowledgeable lactation consultants can be invaluable in navigating these sensitive conversations and transitions. Strategies for setting boundaries and encouraging gradual weaning include:
- Visual Schedules: Using pictures or visual timers to indicate when and for how long breastfeeding will occur.
- Distraction and Substitution: Offering alternative comforting activities, snacks, or drinks when breastfeeding is not an option.
- Verbal Scripts: Consistently using simple, predictable phrases to explain boundaries (e.g., "After we read this book," "Later, when the clock shows…").
- Gradual Reduction: Slowly decreasing the number or length of feeds over time, rather than abrupt cessation.
- Focus on Connection: Ensuring plenty of non-feeding cuddles, playtime, and one-on-one attention to maintain closeness.
Implications and Future Directions

The insights into breastfeeding for autistic parents and children highlight a critical need for systemic changes in maternity and pediatric care. Healthcare providers, including midwives, health visitors, and lactation consultants, require specialized training to understand the nuances of autism, recognize undiagnosed autistic individuals, and adapt their support strategies. This includes a shift towards individualized care plans, offering flexible communication methods, creating sensory-friendly environments, and adopting a trauma-informed approach.
Advocacy groups like the Maternity Autism Research Group (MARG) are pivotal in driving research and raising awareness, ensuring that the unique needs of autistic parents are acknowledged and addressed. Fostering supportive communities, both online and in person, where autistic parents can share experiences and find validation, is also essential.
Ultimately, the goal is to ensure that all parents, regardless of neurotype, have equitable access to compassionate, effective, and tailored breastfeeding support. By embracing neurodiversity and adapting our systems, we can empower autistic parents to achieve their breastfeeding goals, nurture their children effectively, and experience parenthood with greater confidence and well-being. This expanded understanding not only benefits autistic families but enriches the broader tapestry of maternal and child health support, making it more inclusive and responsive to the diverse human experience.

