The journey of breastfeeding, universally recognized for its profound benefits for both parent and child, takes on unique dimensions when intersecting with neurodiversity, specifically autism. As understanding of autism spectrum disorder (ASD) expands, encompassing a broader range of presentations and a greater recognition of autistic adults, particularly women and parents, it becomes increasingly crucial to acknowledge and address the distinct challenges and strengths that arise in the context of lactation. This exploration delves into the nuanced experiences of autistic parents who choose to breastfeed, and parents who are breastfeeding autistic children, advocating for tailored support and a neuro-affirmative approach within maternity and lactation care services.
Understanding Autism in the Context of Parenthood
Autism is a neurodevelopmental difference influencing how individuals perceive the world, interact socially, and communicate. It is understood as a spectrum, meaning its manifestations vary significantly from person to person, and an individual’s abilities and challenges can shift depending on their environment and circumstances. The term "neurodivergent" is often used to describe autistic individuals, highlighting that their neurological processing differs from the predominant "neurotypical" population, rather than being inherently deficient. This perspective shift is vital for fostering inclusive and effective support systems.
While awareness of autism has grown, particularly concerning children, a significant portion of the adult autistic population, especially women, remains undiagnosed. Estimates suggest that while approximately 0.82% of the population in England are formally diagnosed as autistic, up to 72% of the autistic population may be undiagnosed. This diagnostic disparity underscores a critical challenge: many autistic parents may not even be aware of their neurodivergence, making it difficult for them to articulate specific needs or for healthcare providers to offer appropriate, individualized support. This hidden demographic emphasizes the need for a universal approach to care that is flexible and sensitive to a wide array of individual differences, whether formally diagnosed or not.

Breastfeeding for Autistic Parents: Strengths and Unique Considerations
For many autistic women and parents, the decision to breastfeed is approached with a blend of unique strengths and potential challenges. Research indicates that autistic individuals often exhibit a remarkable capacity for in-depth research and independent information gathering. This strength can translate into a highly informed and determined approach to breastfeeding, with parents often possessing extensive knowledge about lactation physiology, infant feeding cues, and potential troubleshooting strategies before the baby even arrives. This dedication can be a significant asset in overcoming initial hurdles.
Beyond the intellectual engagement, many autistic parents report finding profound personal benefits in the act of breastfeeding itself. The repetitive, rhythmic nature of feeding can provide a sense of calm and a structured, quiet time for connection, offering a valuable respite from an often overwhelming world. For some, it is an empowering experience, a testament to their body’s capabilities and their commitment to their child’s well-being. This protected time can become a cherished anchor in the chaotic early days of parenthood.
However, the journey is not without its specific considerations. Autistic parents may encounter unique obstacles within standard maternity and breastfeeding support frameworks.
Communication Differences: Communication styles vary widely among autistic individuals. Some may experience situational mutism, where they are unable to speak in certain stressful or unfamiliar environments, despite being verbal in other contexts. This can make traditional support methods, such as phone helplines or verbal consultations in busy clinics, inaccessible or highly anxiety-provoking. The implication is a critical need for diverse communication options, including written forms, email support, text-based services, visual aids, or even allowing a trusted support person to communicate on their behalf. The availability of resources like La Leche League Great Britain’s (LLLGB) written Help Form is an excellent example of an inclusive approach.

Sensory Sensitivities: Sensory processing differences are a hallmark of autism, where individuals may experience senses (sight, sound, touch, taste, smell, proprioception, interoception) with heightened intensity or reduced awareness. During breastfeeding, this can manifest in various ways:
- Touch: The sensation of a baby latching, suckling, or skin-to-skin contact might be overwhelming or, conversely, barely felt. Nipple sensitivity can be a significant factor.
- Sound: The sounds of a baby crying, gulping, or even the ambient noise of a feeding environment can be distressing.
- Smell/Taste: The baby’s natural scent, the smell of milk, or even lingering odors in a room might be intensely perceived.
- Sight: Bright lights, cluttered environments, or direct eye contact (which some autistic individuals find uncomfortable) can hinder relaxation and bonding during feeding.
- Interoception: Difficulties in recognizing internal bodily signals, such as hunger, thirst, or fullness, can impact a parent’s ability to maintain their own nutritional and hydration needs, which are crucial for milk supply and overall well-being.
Healthcare providers need to be mindful of these sensitivities, suggesting strategies like dim lighting, quiet spaces, specific fabric choices for clothing, or the use of sensory aids (e.g., noise-canceling headphones) to create a more conducive feeding environment.
Accessing Support and Mental Health: Many autistic parents report difficulties in accessing or feeling comfortable in traditional group support settings. Anxiety related to social interactions, navigating unfamiliar environments, or the pressure to mask (suppress autistic traits to appear neurotypical) can deter them from seeking help. The experience of birth itself can be traumatizing for autistic individuals, particularly if they felt a lack of control or encountered insensitive care, contributing to higher rates of Post Traumatic Stress Disorder (PTSD) in the autistic community compared to neurotypical people. This history can further complicate their ability to trust and engage with healthcare systems. Providing clear, visual information about what to expect at support groups, offering one-on-one appointments, or enabling attendance with a support person can significantly reduce barriers. It is essential to recognize that an autistic parent might be struggling internally even if they appear calm, as masking can hide significant distress.
Breastfeeding an Autistic Child: Nuances in Infant Feeding
The considerations surrounding breastfeeding extend to the child’s neurodevelopmental profile. While adult autism diagnosis rates historically lagged, diagnosis rates in children are on the rise, leading to more parents navigating early childhood with an understanding of their child’s neurodivergence.
The World Health Organization (WHO) recommends breastfeeding for two years and beyond, with the natural age of weaning estimated between 2.5 and 7 years. For an autistic or neurodivergent child, breastfeeding can play an exceptionally vital role, extending beyond mere nutrition to encompass comfort, regulation, and a primary means of secure attachment.
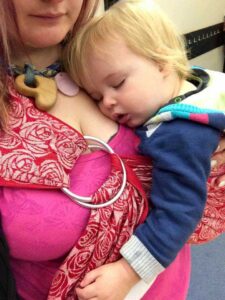
Sensory Differences in Autistic Children: Just like autistic adults, autistic children process sensory input uniquely. This can profoundly impact their feeding experiences:
- Regulation and Comfort: Some autistic children may seek frequent breastfeeding to self-regulate, particularly when overwhelmed by sensory input from their environment (e.g., loud noises, bright lights, new places). Breastfeeding provides a predictable, soothing sensory experience and close physical contact that can help ground them.
- Avoidance: Conversely, strong sensory sensitivities can make feeding difficult. A child might reject breastfeeding due to discomfort with the environment (room temperature, specific smells), or even the texture of their mother’s clothing. Understanding and adjusting the environment to reduce overwhelming sensory input is key.
- Feeding Patterns: These sensory differences can lead to highly individualized feeding patterns. Some children may breastfeed very frequently as a coping mechanism, while others might feed less often due to sensory overload or aversion.
"High Needs" Babies and Parental Self-Care: Many babies, irrespective of neurotype, can be described as "high needs," requiring intense closeness and frequent attention. This can be particularly pronounced in neurodivergent children, whose need for proximity and reassurance can be exceptionally intense. While normal, this intensity can be physically and emotionally demanding on the parent. Emphasizing self-care for parents, encouraging support from family and friends, and connecting with like-minded communities (both neurotypical and neurodivergent-inclusive) are crucial for sustaining breastfeeding relationships, especially during the demanding early years.
Weaning and Boundaries: Weaning from the breast, a significant developmental milestone, can present amplified challenges when an autistic child is involved.
- Sensory and Communication Barriers: Autistic children may struggle with the introduction of solid foods due to sensory aversions to specific textures, tastes, smells, or even the visual appearance of food. This can lead to a prolonged reliance on breastfeeding as a primary source of nutrition and comfort.
- Interoception Issues: Similar to autistic adults, autistic children may have difficulties recognizing hunger or fullness cues, making structured feeding times or boundary-setting complex.
- Co-regulation: Breastfeeding often serves as a primary method for an autistic child to co-regulate their emotions and sensory experiences. Removing this comfort mechanism without adequate alternatives can be highly disruptive.
Parents of autistic toddlers and older children often report a need for more information and support regarding gentle weaning strategies. When parents choose to set boundaries or limit feeds, options can include: - Visual Schedules: Using pictures or social stories to communicate when and where breastfeeding will occur.
- Short Feeds: Gradually reducing the length of feeds.
- Distraction: Offering engaging alternatives when the child seeks to nurse.
- Comfort Alternatives: Replacing nursing with other forms of physical closeness, cuddles, or sensory-friendly activities.
Lactation consultants, like LLL Leaders, can offer invaluable, individualized guidance on navigating these complex weaning processes, respecting both the child’s needs and the parent’s well-being. Continuing to breastfeed into toddlerhood and beyond, especially if a child has a limited diet due to sensory issues, can provide essential nutrients and ongoing immune support.
Implications for Healthcare and Support Systems
The intersection of breastfeeding and autism highlights a critical need for evolving practices within maternity and lactation support services.

- Neuro-Affirmative Training: Healthcare professionals, including midwives, health visitors, and lactation consultants, require comprehensive training in neurodiversity-affirming care. This involves understanding the varied presentations of autism, recognizing potential masking, and approaching care from a strengths-based perspective.
- Individualized Care Plans: A "one-size-fits-all" approach is ineffective. Support must be highly individualized, considering each parent’s and child’s unique sensory profile, communication style, and emotional needs. This may involve longer appointment times, pre-visit questionnaires, or designated quiet spaces.
- Accessibility: Services must enhance accessibility beyond physical ramps. This includes multi-modal communication options, clear and concise written information (perhaps with visual aids), predictable environments, and flexibility in scheduling. Local breastfeeding groups can benefit from providing detailed information about their location, what to expect, and allowing support persons.
- Early Identification and Support: Greater awareness of autism in women and parents could lead to earlier diagnoses or, at the very least, a greater sensitivity from healthcare providers to individual differences that might signal neurodivergence. This proactive approach can significantly improve outcomes and reduce trauma.
- Research and Advocacy: Continued research into the specific experiences of autistic parents and children is vital to inform best practices. Advocacy efforts are needed to ensure that national health policies and funding support inclusive and tailored care for neurodivergent families.
In conclusion, the discourse around breastfeeding and autism underscores the beauty and complexity of human experience. By recognizing the inherent strengths of autistic parents and the unique needs of both autistic parents and children, support systems can evolve to offer truly inclusive, empathetic, and effective care. This approach not only empowers neurodivergent families but also enriches our collective understanding of the diverse tapestry of parenthood. The ultimate goal is to foster an environment where every parent feels seen, heard, and supported in their breastfeeding journey, ensuring the well-being of both parent and child.

